Economic Snapshot for January 28, 2009
COBRA expansion won’t benefit most low-income workers
by Alexander Hertel
A variety of minor changes to COBRA—a federal program that allows recently laid-off workers to continue enrollment with their workplace health insurance for 18 months—have been proposed as part of the economic stimulus package currently under debate. Policy makers, however, should recognize the opportunity to marry the twin goals of greater health security and economic stimulus. To be eligible for COBRA, workers need to have had insurance before being laid-off. Those who worked but did not receive health insurance benefits as well as those who have been out of employment for an extended time will get no help from the proposed COBRA changes.
The figure below demonstrates the extent of this problem. About 63% of workers below 200% of the federal poverty line are ineligible for COBRA benefits compared to only a quarter of workers above that level. COBRA improvements, while important, simply won’t suffice. The COBRA enhancements in current proposals should be supplemented with other ideas for economic stimulus through health care reform, such as expansions to Medicaid and the State Children Health Insurance Program as well as tax credits for employers who cover more of their workforce or ramp up the generosity of their current coverage. Now is no time to think small regarding either health care or economic stimulus.
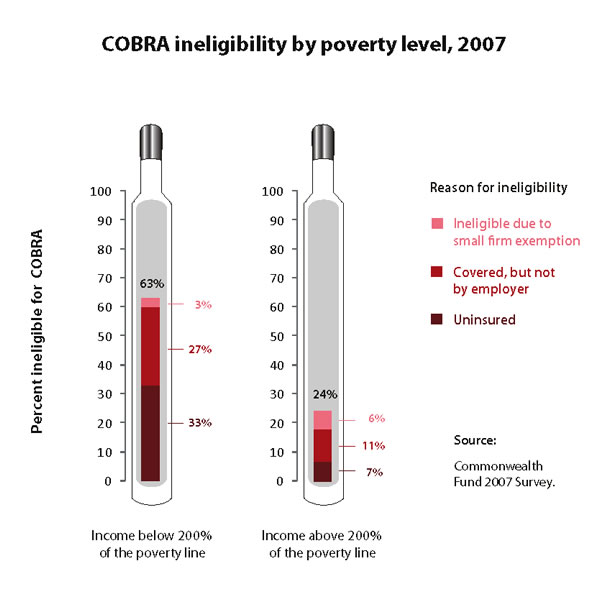
To learn more about the continued erosion of employer-sponsored health insurance, refer to the related briefing paper by EPI Economist Elise Gould:
http://www.epi.org/publications/bp223/
For more information on current utilization of COBRA, and the composition of workers who would likely benefit from the proposed expansions, refer to the recently released Commonwealth Fund Report: Maintaining Health Insurance During a Recession: Likely COBRA Eligibility (2009): http://www.commonwealthfund.org/publications/publications_show.htm?doc_id=784702